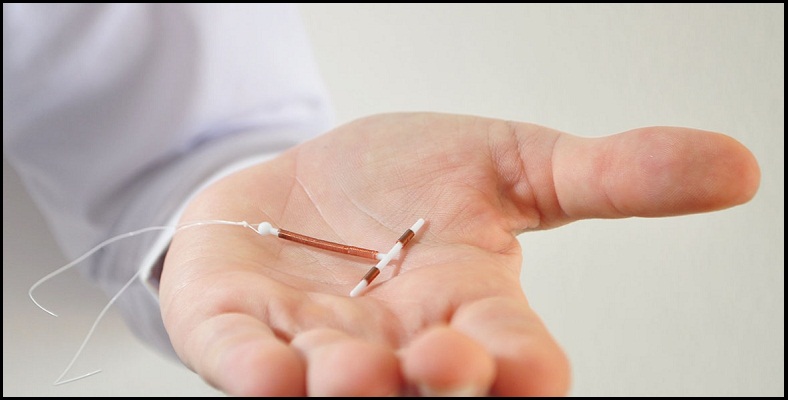
IUD
- Description
- Faq's
Definition:
Mirena is a hormonal intrauterine device (IUD) that's inserted into the uterus for long-term birth control (contraception). A T-shaped plastic frame that releases a type of progestin, Mirena thickens the cervical mucus to prevent sperm from reaching or fertilizing an egg. Mirena also thins the lining of the uterus and partially suppresses ovulation.Mirena is one of two hormonal IUDs with Food and Drug Administration approval. The other is Skyla, which prevents pregnancy for up to three years. Mirena prevents pregnancy for up to five years after insertion.
Why it's done ?
Mirena offers effective, long-term contraception. It can be used in premenopausal women of all ages, including teenagers.
Among various benefits, Mirena:- Eliminates the need to interrupt sex for contraception
- Doesn't require partner participation
- Can remain in place for up to five years
- Can be removed at any time, followed by a quick return to baseline fertility
- Decreases menstrual bleeding after at least several months of use
- Decreases severe menstrual pain and pain related to endometriosis
- Decreases the risk of pelvic inflammatory disease caused by sexually transmitted infections (STIs) by causing the cervical mucus to thicken, creating a barrier against bacteria
- Decreases the risk of endometrial cancer and possibly cervical cancer
- Can be used while breast-feeding — though the recommendation is to wait at least six weeks after childbirth
- Doesn't carry the risk of side effects related to birth control methods containing estrogen
Mirena isn't appropriate for everyone, however. Your health care provider may discourage use of Mirena if you:
- Had or have breast cancer
- Have uterine or cervical cancer
- Have liver disease
- Have uterine abnormalities, such as fibroids, that interfere with the placement or retention of Mirena
- Currently have a pelvic infection or have a history of pelvic inflammatory disease
- Have unexplained vaginal bleeding
- Have inflammation of the vagina or cervix or a lower genital tract infection
- Are allergic to any component of Mirena
- Have or are at high risk of a sexually transmitted infection
In addition, tell your health care provider if you:
- Take any medications, including nonprescription and herbal products
- Have diabetes or high blood pressure
- Have a heart condition or have had a heart attack
- Have migraines
- Have blood-clotting problems or have had a stroke
- Recently gave birth or are breast-feeding
Risks :
Less than 1 percent of women who use Mirena will get pregnant in a year of typical use. If you do conceive while using Mirena, you're at higher risk of an ectopic pregnancy — when the fertilized egg implants outside the uterus, usually in a fallopian tube.
However, because Mirena prevents most pregnancies, women who use it are at lower risk of having an ectopic pregnancy than are other sexually active women who are not using contraception.Mirena doesn't offer protection from sexually transmitted infections (STIs).
Side effects associated with Mirena include:- Headache
- Acne
- Breast tenderness
- Irregular bleeding
- Absence of periods (amenorrhea), especially after one year of use
- Mood changes
- Weight gain
- Ovarian cysts
- Cramping or pelvic pain
It's also possible to expel Mirena from your uterus. You may be more likely to expel Mirena if you:
- Have never been pregnant
- Have heavy or prolonged periods
- Have severe menstrual pain
- Previously expelled an IUD
- Are younger than age 20
- Had Mirena inserted immediately after childbirth or an abortion
After childbirth, your health care provider may recommend that you wait at least eight weeks before having Mirena inserted to avoid possible expulsion.
In addition, your health care provider may recommend removal of Mirena if you develop:
- A pelvic infection
- Inflammation of the endometrium (endometritis)
- Endometrial or cervical cancer
- A significant increase in blood pressure
